Cortisol and Belly Fat After 40: What’s the Connection?
Last Updated: 2026
I used to think my belly fat problem was a diet problem.
For months, I tracked every calorie, eliminated sugar, cut back on wine, and pushed myself to exercise five days a week. The number on the scale barely moved. And what really got to me was that the fat I most wanted to lose — that stubborn, round belly that seemed to appear out of nowhere in my early 40s — was the last thing to go, and often the first thing to come back.
It wasn’t until I had a conversation with a functional medicine doctor that I understood what was actually going on. She asked me one question I hadn’t expected: “How’s your stress level?”
That’s when I started learning about cortisol.
If you’ve been eating well and exercising consistently but your belly just won’t budge, cortisol may be the missing piece of your puzzle. This isn’t a minor footnote in the weight-loss conversation — for women over 40, it’s often central to the whole story.
Quick Navigation
- What Is Cortisol and Why Does It Matter After 40?
- The Direct Link Between Cortisol and Belly Fat
- Why Cortisol Gets Worse After 40 Specifically
- The Hidden Cortisol Triggers You’re Missing
- 10 Science-Backed Ways to Lower Cortisol
- My Daily Cortisol Routine
- FAQ

What Is Cortisol and Why Does It Matter After 40?
Cortisol is your primary stress hormone, produced by the adrenal glands in response to perceived threats — whether that’s a car cutting you off in traffic, a difficult conversation with your teenager, or a deadline at work that has you up at midnight.
In small, short-term doses, cortisol is genuinely helpful. It sharpens your focus, mobilizes energy, suppresses non-essential functions during a crisis, and helps you respond quickly. This is the fight-or-flight response, and it evolved to keep us alive.
The problem is that our modern lives have turned that short-term emergency response into a chronic, low-grade hum that never fully switches off.
For women over 40, this matters in a way that’s different from younger women. As estrogen and progesterone decline during perimenopause, the hormonal buffer that used to soften the cortisol response weakens. Estrogen has a moderating effect on the HPA axis — the hypothalamic-pituitary-adrenal system that regulates cortisol production. As estrogen drops, cortisol can rise more easily, stay elevated longer, and have stronger effects on the body.
This means the same level of stress that felt manageable in your 30s can create a much more significant cortisol spike in your 40s. Your body hasn’t gotten weaker — the hormonal landscape has simply changed.
The Direct Link Between Cortisol and Belly Fat
Here’s what the research tells us, and it’s surprisingly specific.
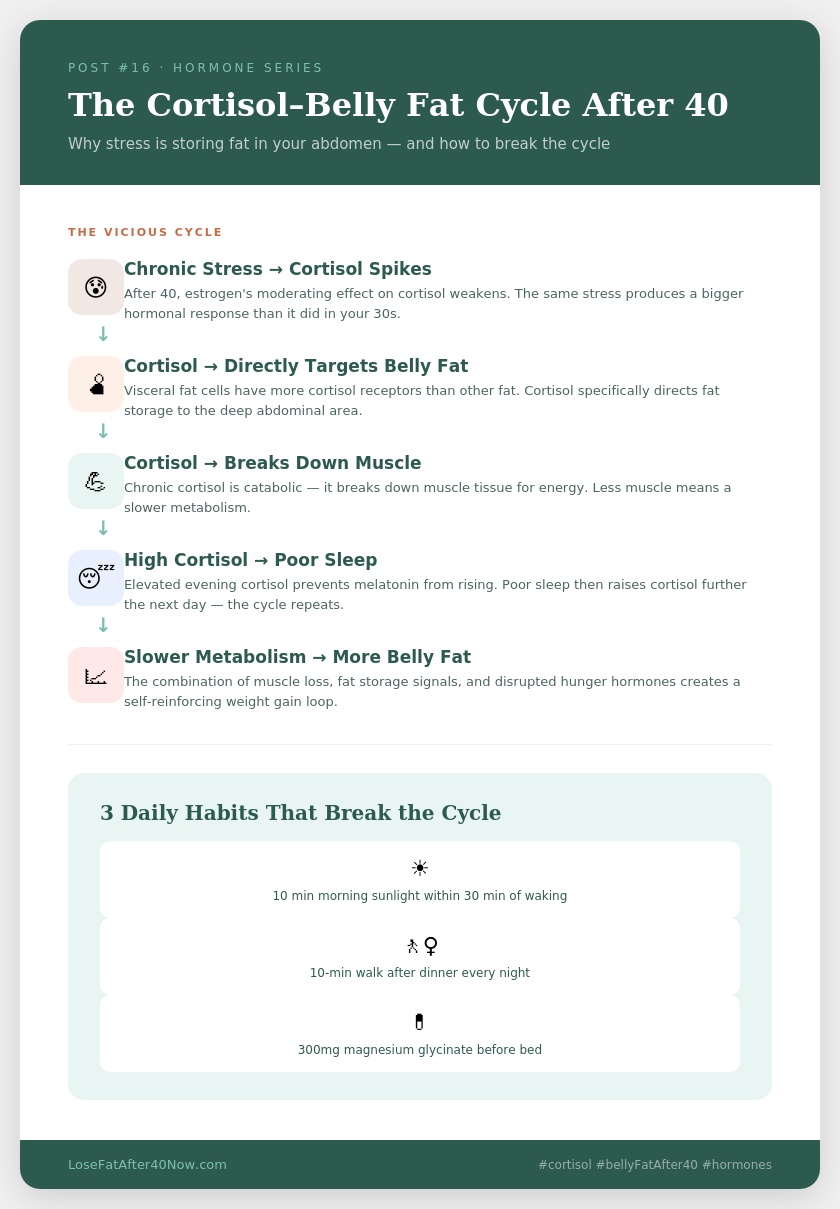
Cortisol doesn’t just promote general fat storage. It specifically drives fat toward visceral adipose tissue — the deep belly fat that surrounds your organs. This isn’t random. Visceral fat is loaded with cortisol receptors, which means it’s especially responsive to cortisol signals. The more chronically elevated your cortisol, the more aggressively your body stores fat in this specific location.
A 2000 study published in Psychosomatic Medicine found that women with greater reactivity to stress (meaning their cortisol spiked more readily) had significantly more abdominal fat — even when controlling for overall body weight. It wasn’t about how much they weighed. It was about where the fat lived, and cortisol was the key factor.
Here’s the mechanism at work:
Cortisol increases appetite — specifically cravings for high-calorie, high-sugar, and high-fat foods. This is your brain looking for fast energy to deal with the perceived threat. Stress-eating isn’t a character flaw. It’s a hormonal response.
Cortisol promotes fat storage by increasing lipoprotein lipase activity in abdominal fat cells. In plain English: it makes your belly fat cells better at absorbing and storing fat from the food you eat.
Cortisol breaks down muscle to use as an energy source during periods of sustained stress. Less muscle means a slower metabolism, which means fewer calories burned at rest — which makes fat loss even harder.
Cortisol disrupts sleep, which then raises cortisol further, creating a self-reinforcing cycle. Poor sleep increases ghrelin (hunger hormone) and decreases leptin (fullness hormone), making you eat more while simultaneously burning fewer calories.
The cruelest part? The things many women do when they’re stressed and trying to lose weight — extreme restriction, intense exercise, skipping meals — can actually raise cortisol further. The body interprets extreme dieting and over-exercising as additional stressors. This is why the harder-is-better approach often backfires in your 40s.
🔗 Related: Hormone Changes After 40: How They Affect Your Weight →
Why Cortisol Gets Worse After 40 Specifically
There are several converging reasons why cortisol becomes a more significant problem in midlife.
Estrogen’s decline removes a buffer. Estrogen has a protective effect on the stress response. It moderates cortisol reactivity and supports the recovery of the HPA axis after a stressor. As estrogen declines, this buffer weakens — and the same life stressors that felt manageable at 35 can now produce a stronger cortisol response.
Life stress tends to peak in your 40s. Think about everything that tends to converge in this decade: career pressures, raising teenagers, supporting aging parents, financial responsibilities, relationship changes. The 40s are genuinely demanding in ways that add up. And the body doesn’t distinguish between emotional stress and physiological stress — it responds to both with cortisol.
Sleep disruption raises cortisol. Perimenopause commonly disrupts sleep through hot flashes, anxiety, and the general restlessness that comes with hormonal fluctuation. Poor sleep is a powerful cortisol trigger, which then makes sleep worse — a cycle that can be difficult to interrupt.
Chronic dieting raises cortisol. Many women arrive at their 40s with years of on-and-off dieting behind them. Severe calorie restriction is a physiological stressor. The body responds to perceived starvation by elevating cortisol — which promotes fat storage as a survival mechanism. The very history of dieting can set up a cortisol pattern that’s hard to break.
🔗 Why the old approaches don’t work: Why Is It So Hard to Lose Weight After 40? →
The Hidden Cortisol Triggers You’re Missing
Most women think about stress in terms of big, obvious events — job loss, divorce, illness. But cortisol responds to many subtler triggers that fly under the radar.
Under-eating. If you’re consuming fewer than 1,200 calories per day, your body likely interprets this as a famine signal. Cortisol rises to mobilize stored energy and preserve survival. The restriction that’s supposed to help you lose fat is actually triggering a cortisol-driven fat-storage response.
Too much high-intensity exercise. This surprised me. I used to think more cardio was always better. But long, intense cardio sessions — particularly on an empty stomach — raise cortisol significantly. After 40, when cortisol is already higher, adding this additional stimulus can counteract the benefits of the workout itself.
Caffeine. A morning coffee is fine for most people. But multiple cups throughout the day, or caffeine consumed after 2 p.m., can keep cortisol elevated well into the evening — disrupting sleep, which then raises cortisol further the next day.
Scrolling before bed. The emotional stimulation of social media, news, or stressful content triggers cortisol just before the period when your body most needs it to drop. Evening cortisol elevation is one of the most significant contributors to poor sleep quality in women over 40.
Inflammatory foods. Ultra-processed foods, refined sugars, and industrial seed oils drive low-grade inflammation — which is itself a physiological stressor that elevates cortisol independently of psychological stress.
Skipping breakfast. Cortisol is naturally highest in the morning (this is what wakes you up). Without food to signal safety and abundance to your body, morning cortisol can stay elevated longer, setting up a reactive hormonal pattern for the rest of the day.

10 Science-Backed Ways to Lower Cortisol After 40
Here’s what I’ve found actually works — based on research, but also based on what has made a measurable difference in my own life.
1. Morning sunlight within 30 minutes of waking.
Light exposure in the morning anchors your cortisol peak early, allowing it to drop naturally throughout the day. This one habit alone can meaningfully shift the cortisol curve over time. Five to ten minutes outside — even on a cloudy day — is enough.
2. Eat breakfast within two hours of waking.
A protein-centered breakfast signals safety and abundance to the body, helping cortisol drop from its morning peak rather than staying elevated. Aim for 25 to 30 grams of protein at breakfast specifically.
3. Walk after meals.
A 10-minute walk after lunch or dinner lowers cortisol directly while also improving blood sugar regulation. This is one of the simplest, most accessible cortisol tools available — and it’s completely free.
4. Reduce high-intensity cardio sessions.
Replace one or two weekly cardio sessions with strength training. Moderate resistance training actually helps regulate cortisol over time, while chronic high-intensity cardio can worsen it. Walking is your cortisol-friendly cardio.
5. Prioritize sleep.
Sleep is genuinely the highest-leverage intervention available. Even small improvements in sleep duration and quality produce measurable reductions in cortisol.
🔗 Sleep strategies: Sleep and Weight Loss After 40: Why 7 Hours Is Non-Negotiable →
6. Magnesium glycinate before bed.
Magnesium supports GABA, the brain’s primary calming neurotransmitter. It directly helps lower evening cortisol and improve sleep quality. 300 to 400mg taken 30 minutes before bed is the standard recommendation.
7. Slow breathing for five minutes.
Physiological sighing — inhale through your nose, then a second quick inhale to fully inflate your lungs, followed by a long slow exhale — has been shown in Stanford research to lower cortisol and activate the parasympathetic nervous system faster than any other known breathing technique. Five minutes is enough.
8. Eat enough protein and food.
Stop undereating. Adequate calorie and protein intake signals to your body that resources are available — which helps bring cortisol down. Severely restricting while also exercising is one of the most effective ways to keep cortisol chronically high.
9. Reduce caffeine after noon.
If you’re experiencing sleep problems and mid-afternoon energy crashes, cutting caffeine after 12 p.m. for two weeks can make a surprising difference in both cortisol rhythm and sleep quality.
10. Cold exposure — carefully.
Brief cold exposure (like ending a shower with 30 seconds of cool water) can help reset the cortisol response over time. Don’t do this if you’re already in a high-stress state — it’s a stressor itself, and the goal is reducing total cortisol load.
My Daily Cortisol Routine
I want to be honest with you: I didn’t implement all of this at once. That would have been its own source of stress.
What I started with was this:
In the morning, I step outside with my coffee for 10 minutes before checking my phone. That’s it. Just 10 minutes of morning light before the day pulls at me.
At dinner, I take a 10-minute walk around the block afterward — rain or shine.
Before bed, I take 300mg of magnesium glycinate and I don’t look at my phone for 30 minutes before sleep.
Three things. That’s what I started with, and those three things genuinely shifted something. My sleep improved within two weeks. My mid-afternoon cortisol crashes lessened. And over the following two months, I started to notice changes in my belly that hadn’t happened despite months of stricter dieting.
I’m not saying cortisol management is magic. Diet and exercise still matter — a lot. But for me, and for many women I’ve heard from, addressing cortisol was the piece that made everything else work better.
🔗 Build the full routine: Daily Routine to Lose Belly Fat After 40 (Simple Habits That Work) →
The Cortisol–Belly Fat Connection: A Summary
| Cortisol Effect | Impact on Belly Fat |
|---|---|
| Increases appetite | More calories consumed |
| Promotes fat storage in abdomen | Direct visceral fat accumulation |
| Breaks down muscle | Slower metabolism |
| Disrupts sleep | More hunger hormones, less fat burning |
| Raises blood sugar | More insulin, more fat storage |
Frequently Asked Questions
Can you test your cortisol levels at home?
Yes — saliva cortisol tests (available online or through some functional medicine providers) can give you a snapshot of your cortisol levels at different times of day. They’re not a substitute for a doctor’s assessment, but they can be a useful starting point if you suspect cortisol dysregulation is playing a role in your weight issues.
How long does it take for cortisol reduction to affect belly fat?
Most women who consistently apply cortisol management strategies notice changes in sleep and energy within 2 to 4 weeks. Visible changes in belly fat typically begin around 6 to 8 weeks, with more significant results at the 3 to 4 month mark. The timeline depends on how elevated cortisol was to begin with.
Can meditation help lower cortisol?
Yes, consistently. Even brief meditation practices — 5 to 10 minutes daily — have been shown in multiple studies to reduce cortisol levels over time. You don’t need a complicated practice. Focusing on your breath for five minutes with your eyes closed is genuinely enough to activate the parasympathetic nervous system.
Does cortisol affect women differently than men?
Yes, meaningfully. Women tend to have a stronger cortisol response to certain types of social stress, and estrogen’s role in moderating cortisol means that the hormonal transition of perimenopause creates specific cortisol vulnerabilities that men don’t face in the same way.
Is cortisol always bad?
No — cortisol is essential. The problem is chronically elevated cortisol, not cortisol itself. The goal isn’t to eliminate stress or suppress cortisol completely. It’s to help the body regulate its cortisol response more effectively so that cortisol rises when needed and drops when it should.
The Bottom Line
Belly fat after 40 is not simply a calories-in, calories-out problem. For many women, cortisol is the invisible force driving fat toward the abdomen regardless of how little they eat or how much they exercise.
Understanding this doesn’t mean giving up on diet and exercise. It means adding a third pillar — stress and cortisol management — to your fat-loss strategy. And it means doing so with compassion for what your body is actually going through during this transition.
You’re not lazy. You’re not broken. You may simply be chronically stressed in ways your biology is amplifying.
Start with morning sunlight and an after-dinner walk this week. Give it a month. See what happens.
Has stress been an invisible factor in your weight loss journey? I’d love to hear your experience in the comments below.
Disclaimer: This post is for informational purposes only and does not constitute medical advice. If you suspect cortisol dysregulation or adrenal issues, please consult with a qualified healthcare provider.




