How Intermittent Fasting Changes After Menopause
Last Updated: May 2026
I want to start with something most intermittent fasting guides won’t tell you.
The version of IF that worked for me at 43 — the 14:10 protocol with an early eating window, moderate coffee, and consistent sleep — stopped feeling the same at 51. Not dramatically. Not overnight. But noticeably.
The brain fog during fasting windows was sharper. My sleep, which had been improving with the protocol, started to fragment again. And the ease with which I’d maintained my eating window started to feel like effort.
I went back to the research, and what I found made immediate sense.
Menopause isn’t just a shift in one hormone — it’s a reorganization of the entire endocrine system. The hormonal context in which intermittent fasting operates changes significantly after your final menstrual period. And the protocol that works brilliantly in perimenopause may need meaningful adjustment on the other side of menopause.
This isn’t a reason to abandon intermittent fasting. The metabolic benefits are real and well-documented, and they may be even more relevant in the postmenopausal years. But understanding how the terrain has shifted is what allows you to adapt intelligently.

What Changes Hormonally After Menopause
To understand how IF needs to change after menopause, it helps to understand what the hormonal landscape actually looks like on the other side.
Estrogen stabilizes at a lower level. During perimenopause, estrogen fluctuates unpredictably. After menopause, it settles into a consistently lower baseline. The estrogen-related benefits — insulin sensitivity support, cortisol moderation, appetite regulation — are consistently reduced rather than intermittently available.
Progesterone is essentially absent. Post-menopause, progesterone levels drop to near zero. This has significant implications for sleep (progesterone promotes GABA, the brain’s primary calming neurotransmitter), cortisol regulation, and gut motility.
Cortisol baseline tends to be higher. With both estrogen and progesterone no longer moderating the HPA axis, the stress response tends to run hotter. Fasting — which is a mild physiological stressor — may produce stronger and more prolonged cortisol responses post-menopause.
Thyroid function often shifts. The menopausal transition is associated with increased risk of thyroid dysfunction, and thyroid hormone interacts with fasting in complex ways. Extended fasting can suppress T3 (active thyroid hormone) in some women.
Insulin resistance often increases. Post-menopause, insulin resistance tends to worsen further, making blood sugar management both more important and more challenging.
How Menopause Affects Fasting Tolerance
These hormonal shifts have concrete, practical implications for how the body experiences fasting.
Longer fasts may feel harder post-menopause. The cortisol response to fasting tends to be stronger without estrogen’s moderating influence. Women who previously fasted 16 hours comfortably may find the same protocol produces more pronounced hunger, brain fog, or irritability post-menopause.
Sleep disruption interacts more severely with fasting. Post-menopausal sleep is often lighter and more fragmented. The cortisol disruption from inadequate sleep compounds with the cortisol elevation from fasting — creating a more challenging hormonal environment.
The tolerance for skipping breakfast decreases. Cortisol is highest in the morning (the cortisol awakening response), and without food to signal abundance and safety, morning cortisol can stay elevated longer in post-menopausal women, affecting mood, cognitive function, and energy for hours.
Recovery from fasting is slower. Post-menopause, with lower estrogen and often lower muscle mass, metabolic flexibility may be less robust, making the adaptation period harder.
The Metabolic Case for IF After Menopause
Despite these challenges, the metabolic rationale for intermittent fasting may actually be stronger post-menopause than before — if done appropriately.
Insulin resistance is the primary metabolic challenge post-menopause. Without estrogen’s support for insulin sensitivity, post-menopausal women face meaningfully higher insulin resistance. This is the direct driver of belly fat accumulation, blood sugar dysregulation, and metabolic syndrome risk. Intermittent fasting — by extending the periods when insulin levels are low — directly addresses insulin resistance at its root.
A 2022 study published in Obesity found that time-restricted eating in post-menopausal women produced significant reductions in insulin resistance, visceral fat, and inflammatory markers over 12 weeks, with greater effects than calorie restriction alone.
Autophagy becomes more valuable with age. Autophagy — the cellular cleanup process triggered by fasting — becomes progressively more important as we age. Fasting windows of 14+ hours trigger meaningful autophagy that supports cellular health in ways that matter more, not less, as we get older.
Blood sugar management is more critical. Intermittent fasting, by reducing the total number of meals and naturally limiting refined carbohydrate opportunities, is one of the most effective tools for managing post-meal blood sugar spikes.
How to Modify Your IF Protocol Post-Menopause
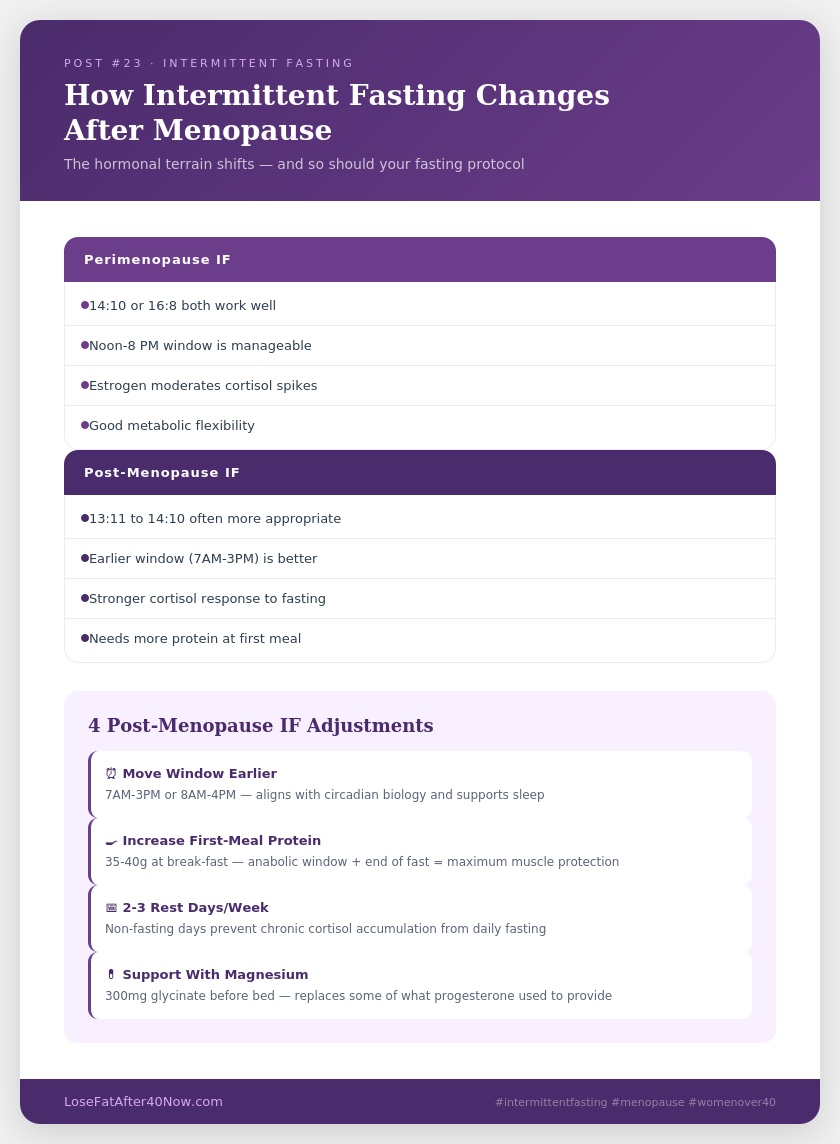
Shorten the fasting window if needed. If you’ve been doing 16:8 comfortably and it still works, continue. But if sleep is fragmenting, brain fog is worsening, or mood is unstable during fasting, shortening to 14:10 or even 13:11 is not a step backward — it’s an intelligent adaptation to your hormonal reality.
Move the eating window earlier. This is the single most important adjustment for post-menopausal women. An eating window of 7 AM to 3 PM or 8 AM to 4 PM — called early time-restricted eating (eTRE) — produces significantly better insulin sensitivity and sleep outcomes than a later window (e.g., noon to 8 PM).
Prioritize protein at your first meal. After a fasting window, muscle protein synthesis is most responsive. A first meal containing 35-40 grams of protein directly after the fasting window is more important than it was in earlier years.
Take 2-3 non-fasting days per week. Two or three days per week where you simply eat normally (3 balanced meals without specific timing restrictions) reduces the chronic cortisol load while preserving the metabolic benefits of the fasting days.
Support fasting with magnesium and sleep. Magnesium glycinate (300-400mg before bed) directly supports the cortisol regulation and GABA function that progesterone used to provide.
The Early Eating Window Advantage
Traditional IF advice often places the eating window in the middle of the day or later (noon to 8 PM being a common recommendation). For post-menopausal women, this turns out to be suboptimal.
Insulin sensitivity is highest in the morning. Your body is most equipped to handle carbohydrates earlier in the day. Eating a larger portion of your calories — particularly carbohydrates — in the morning and tapering toward a lighter, earlier dinner aligns with this biological reality.
Cortisol is highest in the morning and should drop through the day. Eating early signals safety to the body, supports the cortisol drop, and allows melatonin to rise naturally in the evening, supporting sleep quality.
| Time | Meal |
|---|---|
| 7:00–8:00 AM | First meal: High protein (35-40g), moderate fat, some complex carb |
| 12:00–1:00 PM | Second meal: Protein + vegetables + healthy fat |
| 3:00–4:00 PM | Third meal (light): Protein + vegetables, minimal carbohydrate |
| 4:00 PM onwards | Fasting window begins |

Signs Your Current IF Protocol Isn’t Working Post-Menopause
Honest self-assessment is crucial. Here are the signals that your current fasting approach needs adjustment:
- Sleep is getting worse, not better
- Brain fog during fasting windows is intensifying rather than easing
- Hunger feels more urgent and harder to manage than it used to
- Mood during fasting hours is significantly worse than on non-fasting days
- You’re consistently more stressed or irritable
- Your hair is thinning faster than expected
- Body composition isn’t improving despite adherence
If three or more of these resonate, the protocol needs modification — not more willpower.
Rebuilding an IF Approach That Works Now
Start with 13:11. Finish dinner by 7 PM. Eat breakfast at 8 AM. This creates a 13-hour fasting window that produces meaningful metabolic benefits with minimal cortisol cost.
Try this for 3-4 weeks. Assess: How’s your sleep? Energy? Hunger? Brain fog? Mood? If all are stable or improving, you can gradually extend to 14:10.
Keep 2-3 rest days per week. On non-fasting days, simply eat 3 balanced meals at regular times. This is not “breaking” your protocol — it’s protecting your hormonal balance.
Make your first meal protein-first. 35-40g of protein at your first meal of the day. Every time.
Prioritize the ecosystem. Fasting works best when sleep is adequate, strength training is consistent, and stress is managed. The protocol is a tool, not a mandate.
Frequently Asked Questions
Can intermittent fasting help with postmenopausal weight gain?
Yes — particularly by addressing insulin resistance, the primary metabolic challenge post-menopause. Research consistently shows that time-restricted eating improves insulin sensitivity, reduces visceral fat, and lowers inflammatory markers in post-menopausal women. The key is the protocol modification described above: shorter windows, earlier timing, adequate protein.
Is intermittent fasting safe for post-menopausal women with osteoporosis?
This requires individual medical guidance. The potential concern is that fasting may affect calcium absorption timing and bone-related hormones. Women with significant bone density concerns should discuss any significant dietary changes with their healthcare provider.
Does the eating window timing really matter, or is it about total fasting hours?
Research increasingly suggests that timing matters significantly — not just total fasting duration. The alignment between your eating window and your circadian rhythm produces metabolic benefits beyond what fasting duration alone explains. This is especially relevant post-menopause.
What about women on HRT — does IF work differently?
Women on hormone replacement therapy may find that the perimenopausal IF approach works well post-menopause too, because HRT restores some of the hormonal context that makes standard 16:8 more tolerable. However, the early eating window advantage appears to persist regardless of HRT status.
The Bottom Line
Menopause changes the hormonal terrain in ways that matter for intermittent fasting — but they don’t make it contraindicated or ineffective. They make it an adaptation problem.
The woman who thrived on 16:8 from noon to 8 PM at 44 might find that 14:10 from 7 AM to 5 PM serves her better at 52. Both are intermittent fasting. Both provide metabolic benefits. One is aligned with her current hormonal reality, and one isn’t.
Listen to your body. Track your sleep, mood, energy, and hunger during fasting. Adjust based on what you observe, not what a protocol tells you to feel.
How has your experience with intermittent fasting changed around menopause? I’d genuinely love to hear in the comments below.
Disclaimer: This post is for informational purposes only and does not constitute medical advice. Please consult with a qualified healthcare provider before making significant dietary changes, especially if you have existing health conditions.





